Severe Traumatic Injury of the 3rd Cranial Nerve A Case Study by Shmuel Halevi Ph.D |
Severe Traumatic Injury of the 3rd Cranial Nerve A Case Study by Shmuel Halevi Ph.D |
Originally published in the Journal of Chinese Medicine in England (June 2016).
Abstract
In the following case history, acupuncture was used to successfully treat severe damage to the third cranial nerve (and possibly the optic nerve) in a 70 year-old male, which had been caused by traumatic injury. There was considerable probability that without treatment the damage to the nerve would not be reversed. This is the third case study on severe eye disorders been cured solely by acupuncture published by the author. In all of these cases, acupuncture was shown to be superior to conventional medicine, which did not provide any clinical solution.
Foreword
This case history involves a dear friend of mine, who is now at the age of 70. We have been friends since childhood and were born in the same town in Israel. I consider this case the highlight of my 35 years of professional work as a Chinese medicine practitioner. In this peculiar case I used some special approaches and needle techniques, which I thought might be of interest to clinicians who lack experience in treating severe eye disorders with acupuncture. Readers of my articles on my website 1 or in the Journal of Chinese Medicine, will know that I have treated with excellent results eye disorders that had received a very poor biomedical prognosis. The following case makes an excellent addition to those cases, emphasising the great advantages of acupuncture over modern scientific medical options.
Introduction
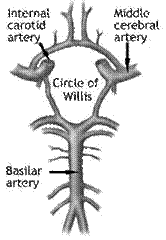
On 10th December 2015 I received a call from M., a dear old friend of mine. His voice on the phone was weak and hoarse and I could barely understand him. This was very unlike him. ‘What happened to you?’ I asked in alarm. ‘I am at the Ichilov - Tel Aviv Sourasky Medical Center, in the eye department. I am in a very bad situation,’ he reported. A few days earlier M. had received several tooth implants at his dentist’s. The procedure had lasted many hours until completion. That very night, M. woke up at around midnight to use the bathroom. He stood up and immediately lost consciousness, falling awkwardly and catching his right ear lobe on the bedpost and almost completely tearing his outer ear in the process. Luckily his wife and daughter heard the turmoil and managed to revive him, and called an ambulance to take him to the nearby hospital. When M. regained consciousness, he discovered to his dismay that he could not focus his eyesight. His left eye now had a severe horizontal strabismus (squint) towards the lateral corner, and there had been significant deterioration in his visual acuity, especially of the left eye. There was also double vision, marked lid droop (ptosis) of the left eye, and he found it difficult to manage the movement of his right eye. Upon his arrival, M. was admitted for emergency stitching of his severed outer ear, and an MRI scan was taken. During the following week M. was hospitalised, and the professor of the eye department established a diagnosis of acute damage to the third cranial nerve, and possibly the optic nerve as well. There was also a critical three millimetre stenosis of the basilar artery 2, which had possibly caused the minor cerebrovascular accident that caused the fall. M. suffered from constant dizziness, general weakness, disorientation and anxiety. This was not the M. who I knew so well - a robust, confident man who woke up early every morning for his seven-mile walk. In view of his doctors’ poor prognosis, M. asked me whether acupuncture could be of any value in his case. I assured him that if treatment was initiated close to the onset of the damage, acupuncture might be the only treatment modality to help him regain functionality in the damaged nerves.
Thus we agreed that as soon as his doctors had concluded their tests, his family would drive him to my clinic in Nahariya, some 160 kilometres north of Tel-Aviv. He would live in my clinic in Nahariya, where I had a spare bedroom, kitchen and bathroom, and his children would take shifts to take care of him at the apartment. I told M. that treatment would be on a daily basis, which was the only option for clinical success in such a case.
Diagnosis
When he arrived, M. appeared to be in a very poor condition. His gait was insecure, and he needed to lean on somebody in order not to trip and fall. He exhibited severe strabismus of the left eye. His left lid drooped, covering his left eye almost completely, and he complained of double vision. M. looked confused and weak. The stitches on his right ear bulged and looked inflamed. He said the ear caused him pain but he considered this his least concern. His pulse was regular and forceful. Both cun positions were wiry and choppy. The Liver position was also quite wiry. His tongue looked somewhat swollen, with a thin yellowish coating. Both Fengchi GB-20 points were abnormally tender, and there were other tender ashi points, particularly surrounding the left eye. These findings were absolutely in accord with the symptoms. They were shi (excess) in nature, and thus confirmed an excess condition. I was relieved. More often than not, findings that are in accord with symptoms have a better prognosis than those that do not. In my experience, a shi condition - especially when due to traumatic injury and where treatment is initiated immediately - has better odds of successful resolution. On the other hand, a shi condition with a long history will tend to establish itself in the body and in time deteriorate into a xu (deficient)- chronic condition – this is much harder to treat. In view of the findings of the MRI scan, I came to the conclusion that the many hours that my friend had spent on the dentist’s chair resulted in pressure over the occipital region. This prolonged pressure hindered the proper flow of qi and blood to the brain, which aggravated the already partially clogged basilary artery. This haemo-dynamic hindrance had come to a climax at midnight, when blood flow is markedly decelerated anyhow. Thus, when M. got up for the bathroom, he abruptly lost consciousness and fell down, bumping the right side of his head on the edge of the bed and floor.
The Treatment Plan and Conception
Laying aside the biomedical diagnosis, as I usually do prior to Chinese medicine treatment, I concluded that this was primarily a case of severe blood stasis. The trauma that preceded the event, i.e. the blow to the head and ear causing the immediate squint of both eyes, loss of eye coordination and abrupt droop of the left eyelid all pointed to this conclusion. The pulse, which was shi and wiry at both cun positions and the Liver position, also pointed to a shi condition involving pain. In addition, the tender Fengchi GB-20 points also supported this conclusion. A shi traumatic injury of this nature calls for strong stimulation, to the maximum extent of the patient’s tolerance, both in terms of needle manipulation and treatment frequency. I delineated all this to my friend, and gained his approval to whatever I saw fit. In view of this, I thus established the following principles of treatment:
· Disperse Qi and Blood in the left eye region using local and distant points.
· Activate upward Qi in order to lift the drooped eyelid.
· Reinforce Qi and Blood in order to regain vitality and will-power.
· Relax shen and relieve anxiety.
Owing to my patient’s underlying weak condition, I decided to commence with milder stimulation and an emphasis on relieving anxiety and circulating qi. Later on, when his overall condition improved, I planned to upscale the intensity of stimulation to put the emphasis on invigorating the blood.
Treatment
The first few treatments included the following point selections:
This treatment plan was carried out daily for one week for one 30-minute session. Along with the needling, I taught my friend how to perform qigong self-massage. This consisted of vigorously massaging both sides of the nose, both eyebrows in medial to lateral strokes, the occipital region and the temples. He carried this out a few times a day until his entire head felt warm. At the end of the first week a great overall improvement had occurred. The patient could walk with much more confidence. He said that, when he concentrated, he could now focus his eyesight on objects. His spirits improved dramatically, and he stopped looking so desperate and agonised. However, there had not been any apparent change in his strabismus or ptosis. At this stage I changed both the point selection and the needling technique, as follows:
Using this new selection of points with a more robust manipulation was intended to shift the emphasis of treatments towards a more aggressive stimulation of qi and blood, vigorous blood dispersion, and the restoration of proper equilibrium at the site of the trauma. There are a few aspects of the point manipulation utilised during this phase that I would like to elaborate on. The first was the application of Zanzhu BL-2 in order to restore the proper tonus and position of my patient’s left eyelid. With due modesty, I claim this technique for ptosis as my personal innovation. I have had outstanding clinical success using this technique in the treatment of this condition. Therefore, I am sharing this knowledge here for the benefit of all. The procedure is as follows: insert a short needle into Zanzhu BL-2 and manipulate it to achieve deqi travelling towards the eye. This should be easily obtainable. The next step, however, is somewhat painful, and the patient should be advised of this. If the patient is of the delicate type or intolerant of physical pain, do not use this technique. Luckily, M. was neither. With the needle in situ, start rotating the shaft slowly clockwise, to entangle the skin around the needle and thus obtain good traction. Then pull the shaft upward a few millimetres and swiftly attach the needle shaft to the skin of the forehead with adhesive tape. This technique, as said before, has a dramatic effect on raising the qi upward in the case of drooping eyelid.
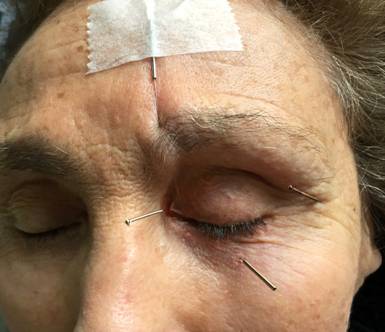
Figure 1: The ‘lid-lift’ technique using Zanzhu BL-2
The second technique relates to the use of the so-called ‘dangerous’ points Jingming BL-1 and Qiuhou (M-HN-8). First, it is advisable to warn the patient that these points (as well as Chengqi ST-1) bear some risk of causing a black eye. However, despite the fact that this is not a pretty sight, it bears no danger and the haematoma usually subsides in a few days. A short and thin needle should be swiftly inserted into one of the points using a guide tube. Thereafter, the practitioner should guide the needle deeper and deeper, while pushing the eyeball gently away using the other hand. Proper qi sensation usually appears at a depth of one cun. Many practitioners refrain from using these points, in view of their anatomical complexity. Those who do use them often refrain from reaching the therapeutic depth for fear of causing damage. However, my experience is that proper use of these points can in some cases make the difference between blindness and a cure.6
The last needle technique I wish to highlight is the use of Zusanli ST-36 in the context of this case. This manipulation is more complicated than those described above and involves skillful handling of the needle in order to be applied properly. When puncturing Zusanli ST-36, there is often a sore sensation - sometimes electric shocklike - that travels along the shin towards the dorsum of the foot. This phenomenon relates to the fact that ST- 36 Zusanli is situated close to the peroneal nerve, and also to the fact that the Stomach channel flows distally towards the foot. Owing to these facts, it can be difficult to propagate qi sensation proximally. In order to do so, we must avoid the peroneal nerve and maintain a very light sensation of deqi at the point by lightly twirling the needle in both directions, while simultaneously massaging the channel proximally until the patient reports the sensation of qi traveling superiorly. It is advisable to encourage the patient to participate in this process by using their mind to in ‘capture’ the qi sensation and guide it proximally to the desired location (in this case the eye). Zusanli ST- 36 is probably the most powerful point of the yangming system, along with Hegu L.I.-4 on the hand. After only a few daily sessions of provoking this type of deqi at Zusanli ST-36, there was no longer a need for the whole procedure. Immediately after needle insertion at the point, M. would report the familiar warm sensation as if liquid was flowing under his skin, traversing the thigh and the abdomen, and arriving eventually at his left eye.
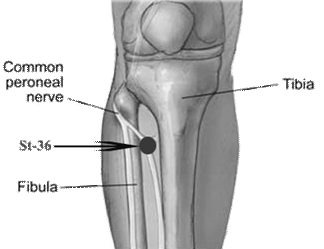
Figure 2: Zusanli ST-36 and the peroneal nerve
The Treatment and its Outcome
After starting the second phase of my treatment plan, positive changes occurred quite rapidly. After only five sessions utilising the ‘lid-lift’ technique at Zanzhu BL-2, M.’s eyelid started climbing back to its proper position. Along with this, he reported the cessation of double vision. In fact, his left eyesight had improved to a degree that he swore it was better than before the accident had occurred. At around the 12th session his squint had greatly improved, and at times would vanish for a considerable number of minutes at a time. He had started taking long walks to the beach by himself and his optimism returned. It is worth mentioning that during this phase I had no real need to provoke the qi to travel in the desired direction. At the moment deqi was obtained, M. felt it flowing along the desired course. This was the case with Zusanli ST- 36 towards the head, as well as with Guangming GB-37 along the left ribcage to the armpit and temple. It should be noted that my friend had no preliminary experience of acupuncture, nor any knowledge of Chinese medicine or the channel system at all. My friend remained at the clinic for fifteen days and received a total of 15 treatments. He was advised to continue qigong self-massage, as well as refrain from coffee 7, cold beverages and losing his temper. His condition continued to improve quickly by itself, and at the time of writing, about three months after this traumatic incident, he is completely cured. M. reports that neurologists and eye doctors who have examined him at the Ichilov - Tel Aviv Sourasky Medical Center are dumbfounded at the progress he made in such a short time.
Footnotes:
1. See <http://www.acumedico.com/eye1.htm> and <http:// www.acumedico.com/eye2. htm>
2. ‘The basilar artery arises from the confluence of the two vertebral arteries at the junction between the medulla oblongata and the pons between the VIth cranial nerves. It ascends superiorly in the central gutter (sulcus basilaris) ventral to the pons and divides at the pontomesencephalic junction into the paired posterior cerebral arteries close to the pituitary stalk.’ (see https://en.wikipedia.org/ wiki/Basilar_artery)
3. According to the Spiritual Pivot ‘The Yangming channel is abundant in qi and blood”. Points of both the arm and leg portions of Yangming channel are therefore much used clinically to regulate qi and blood in the limbs and treat atrophy disorder and painful obstruction, hemiplegia and pain of all kinds.’ In Deadman, P., Al-Khafaji, M. & Baker, K. (1998). A Manual of Acupuncture. Journal of Chinese Medicine Publications: Hove
4. See Chen, J.R. & Wang, N. (1988). Acupuncture Case Histories from China. Eastland Press: Seattle, pp. 220, 253, 271 as well as many other pages.
5. ‘As we know, the primary Yang channels are connected to the primary Yin channels in a Yin/Yang relationship. By combining a point on a Yang channel with another on its paired Yin channel, the cumulative effect is greater than needling either point separately. Examples: combining ST 36 (Zusanli) on the stomach channel (Yang) with SP 4 (Gongsun) on the spleen channel (Yin) for stomach disease. Or, combining L 9 (Taiyuan) on the lung channel (Yin) with LI 4 (Hequ) on the large intestine channel (Yang) for coughing. The most well known combinations of this kind are between the Source points on the channel primarily affected by a disease, and the Connecting point on the channel paired with the first, in the Yin Yang relationship. In this combination the Source point is called the “host” and the Connecting point the “guest”.’ In Shanghai College of Traditional Medicine (1981). Acupuncture: A Comprehensive Text. Eastland Press: Chicago, p.58. This principle of combining points has created renowned combinations such as Hegu L.I.-4 with Lieque LU-7 for upper respiratory tract ailments, Taichong LIV-3 with Guangming GB-37 for eye disorders, Taiyuan LU-9 with Pianli LI-6 for cough caused by phlegm, etc. In addition: ‘The idea behind this form of combination is to divert excess energy from the diseased organ to its parallel Yin/Yang related channel. Thus, by puncturing the “host” point, which is a Source point, one directly drains an overactive organ (Source points are in close relation with their organ). The stimulation of the Luo point of the parallel meridian ensures that the excess Qi would thus leave by the closest possible gate.’ In Chen, J.R. & Wang, N. (1988). Acupuncture Case Histories from China. Eastland Press: Seattle, p. 6-7.
6. See http://www.acumedico. com/eye1.htm
7. In my clinical practice I have ascertained innumerable times the hazardous influence of coffee drinking on the Liver system. I have also been able to demonstrate on several occasions that most people who drink coffee regularly tend to develop a wiry pulse at the Liver position. Moreover, many patients whom I have treated for various medical problems evolving from a Liver condition reported a sudden improvement of their condition when they gave up drinking coffee. In most cases involving a wiry Liver pulse, abstaining from coffee will change this quality to normal in a short period of time as long as there is no other pathological process going on in this organ.